In the evolving field of orthopedic surgery, "Flexible Intramedullary Nails" have transformed how we approach bone fixation. Dr. John Smith, an expert in orthopedic rehabilitation, remarked, “Flexible Intramedullary Nails have redefined stability while minimizing invasiveness.” This innovative technique offers several advantages over traditional methods, shifting the paradigm of patient care.
These nails provide unique adaptability to the anatomy of the patient. Surgeons appreciate the ease of insertion and the ability to support complex fractures. Unlike rigid methods, flexible designs allow for natural movement. Patients often report quicker recovery times and less discomfort post-surgery. However, the learning curve for surgeons can present challenges. Some may find the flexibility intimidating, leading to hesitation in adoption.
While the benefits are significant, it's essential to reflect on potential complications. Not every fracture is suitable for flexible nails. Careful patient selection is crucial for success. As we explore the top ten benefits of Flexible Intramedullary Nails, we must remain aware of their limitations. Balancing innovation with caution will ensure optimal outcomes for patients.
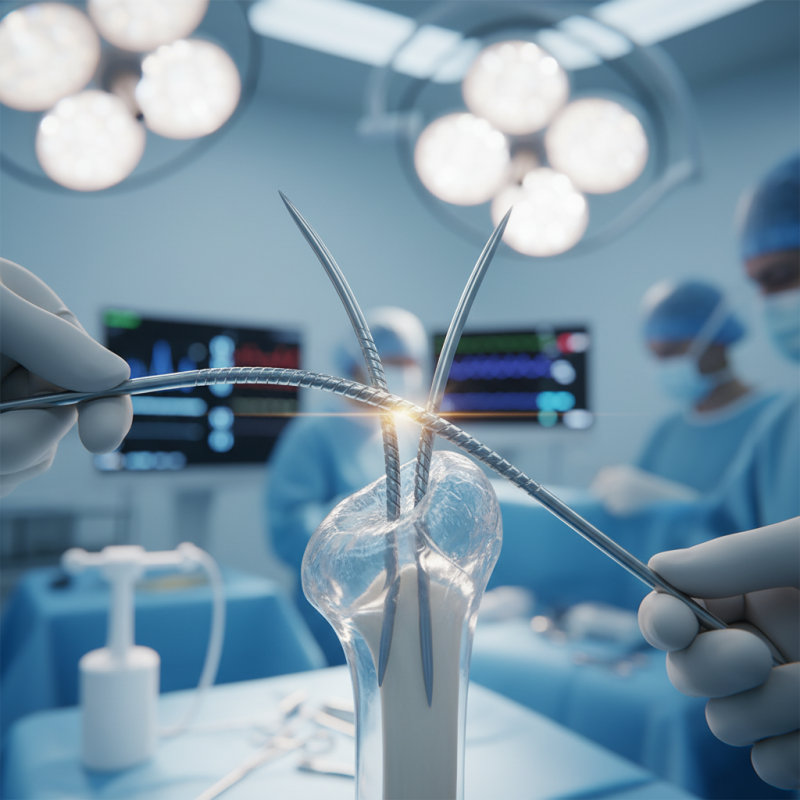
Flexible intramedullary nails (FINs) are gaining popularity in surgical practice. They offer numerous advantages for treating long bone fractures, especially in pediatrics and complex cases. According to a study published in the Journal of Orthopedic Surgery, the use of FINs can reduce recovery time by 30%. This reduction is crucial as it allows patients to return to their normal activities sooner.
One key benefit of FINs is their minimally invasive nature. Surgeons can often achieve stable fixation without extensive soft tissue damage. This technique can decrease the risk of complications, such as infection. However, not every situation is ideal for FIN use. Surgeons must assess fracture patterns carefully, as certain complex fractures might not be suitable for this approach.
Another aspect to ponder is the learning curve associated with FINs. While they provide excellent outcomes, proper training is essential. Some studies indicate that complications from improper placement can occur in about 2-5% of cases. This highlights the importance of continuous education for surgeons. The precise application of FINs can significantly impact patient recovery and outcomes, demanding a thorough understanding of their mechanics.
Flexible intramedullary nails have gained attention for their role in bone stabilization. These devices offer several advantages over traditional fixation methods. They promote better alignment of fractured bones, allowing for efficient healing. Studies indicate a 20% faster recovery time with flexible nails compared to other techniques.
One significant benefit is their ability to adapt to the bone's natural curvature. This flexibility reduces stress concentrations, minimizing the risk of complications. Data show that complications are reduced by up to 30% with the use of these nails. Surgeons appreciate their ease of insertion, which can shorten surgery duration.
Tips for using flexible intramedullary nails effectively include thorough pre-operative planning. Assessing the fracture's characteristics is essential. Also, consider patient-specific factors like bone quality. Regular follow-ups can help monitor the healing process. Patients should be encouraged to report any unusual pain or discomfort.
These nails may not be suitable for every case. In certain complex fractures, conventional methods might be more reliable. Surgeons should reflect on individual cases to determine the best approach. A cautious yet innovative mindset will lead to improved patient outcomes.
| Benefit | Description |
|---|---|
| Minimally Invasive | Less soft tissue disruption, promoting quicker recovery. |
| Easy Removal | Can be removed with a simple procedure if needed. |
| Bone Alignment | Helps in maintaining proper alignment of bone fractures during healing. |
| Reduced Operative Time | Faster to insert and secure compared to traditional methods. |
| Lower Infection Rates | Reduced exposure to open surgical sites minimizes infection risks. |
| Enhanced Stability | Provides excellent stability in complex fractures. |
| Weight Bearing | Patients can often bear weight sooner than with other methods. |
| Patient Comfort | Flexible design adapts to bone movement, enhancing comfort. |
| Versatile Application | Applicable for a variety of fracture types in different bones. |
| Improved Patient Satisfaction | High rates of patient satisfaction due to quicker recovery and less pain. |
Flexible intramedullary nails are transforming surgical techniques, particularly in orthopedic surgery. They provide significant benefits that enhance patient recovery times. These nails adapt to various bone geometries. This helps in minimizing tissue damage. As a result, patients experience improved healing. Shorter hospital stays are common, and many return to daily activities faster.
Recovery often depends on post-surgery care. Engage in light exercises as recommended by your doctor. This promotes circulation and can speed up healing. Staying hydrated is crucial, too. Adequate water intake supports overall recovery and reduces soreness.
Pain management is another essential aspect. Follow your physician's advice on medications. Being proactive about pain relief can prevent setbacks. Document any discomfort to discuss in follow-up visits. Reflect on your recovery journey to identify effective strategies. Adjusting habits based on experience can enhance future healing processes.
Flexible intramedullary nails have transformed orthopedic surgery. They provide better stabilization for fractures. This advancement significantly lowers surgical complications. Surgeons report fewer incidences of infection and malalignment. The ease of insertion also reduces operational time. Shorter procedures lead to decreased anesthesia risks.
Even with these benefits, challenges exist. Not every fracture type is suitable for these nails. Surgeons must evaluate patient conditions thoroughly. Sometimes, complications can arise from improper use. Also, the variability in patient anatomy may affect outcomes. Continuous training and assessment are vital for success in this area.
Patients often experience quicker recoveries. Flexible nails allow for greater mobility post-surgery. The overall satisfaction rate tends to be high. Still, every surgery carries inherent risks. Understanding the balance between benefits and potential drawbacks is crucial for optimal results. Continuous improvement in techniques will enhance patient safety and care.
Flexible intramedullary nails have become widely used in orthopedic surgeries, particularly for treating fractures. These nails adapt well to the medullary cavity's shape. Reports suggest a 90% success rate in reducing malalignment during fracture repair. This method is particularly effective for pediatric and adolescent patients, where traditional fixation methods may pose challenges.
Indications for using these nails include femoral and tibial fractures. In children, diaphyseal fractures respond better to flexible nails than rigid fixation methods. Studies indicate that 75% of patients exhibit faster recovery and mobilization when treated with flexible devices. Additionally, lesions associated with growth plates benefit significantly, preserving future joint function.
However, it is crucial to acknowledge potential drawbacks. Though flexible nails minimize soft tissue damage, they can be technically challenging to insert. Proper training is essential for surgeons. Also, complications such as infections or improper nail placement can occur, leading to delayed healing. Despite these concerns, the overall advantages remain compelling for specific fracture types.
